Introduction
In the realm of medical mysteries, Fahr’s Syndrome stands as a curious enigma that has baffled researchers and clinicians alike. This rare brain disease, characterized by the abnormal accumulation of calcium in the basal ganglia and other brain regions, presents a complex array of challenges for both patients and healthcare professionals.
In this comprehensive article, we will delve into the depths of Fahr’s Syndrome, exploring its origins, manifestations, treatment avenues, and the resilience displayed by those living with this condition.
What is Fahr’s Syndrome?
Fahr’s Syndrome, also known as Fahr’s disease or idiopathic basal ganglia calcification, is a neurodegenerative disorder that involves the progressive deposition of calcium in the brain’s basal ganglia, thalamus, and other regions responsible for movement control and cognitive function.
Initially described by German neurologist Karl Theodor Fahr in 1930, this condition often remains asymptomatic in its early stages, making its diagnosis a daunting challenge.
Causes and Risk Factors of Fahr’s Syndrome
While the exact cause of this condition remains elusive, there are notable factors that appear to contribute to its development. Genetic predisposition has been identified as a potential influencer, with some cases showing a familial pattern.
Additionally, metabolic imbalances and hormonal dysfunction could play a role in the abnormal calcium deposition process. Understanding these factors can pave the way for early identification and intervention.
Symptoms and Diagnosis of Fahr’s Syndrome
The symptoms of Fahr’s Syndrome can vary widely, encompassing both motor and cognitive disturbances. Movement issues such as tremors, muscle stiffness, and gait abnormalities can emerge, along with cognitive impairments including memory loss and executive function deficits.
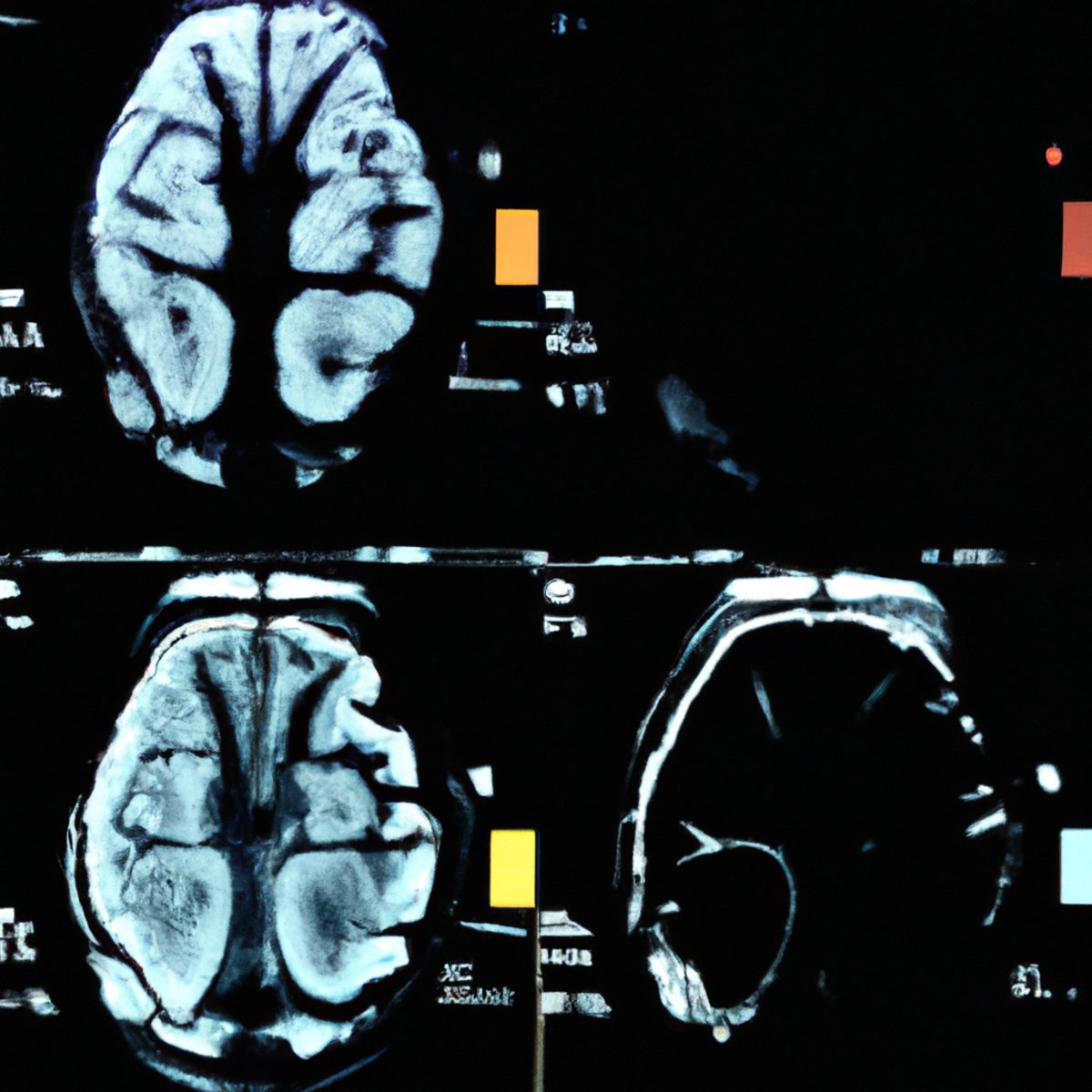
Diagnosing this condition involves a combination of clinical evaluation, neuroimaging techniques like CT scans, and ruling out other conditions that might mimic its symptoms.
Treatment Options for Fahr’s Syndrome
As of now, there is no specific cure for this condition, underscoring the importance of focusing on symptom management and improving the quality of life for affected individuals. Medications can help address some of the motor and cognitive symptoms, while physical and occupational therapies offer valuable support in maintaining functional independence.
A multidisciplinary approach involving neurologists, therapists, and social workers is crucial for devising a comprehensive treatment plan.
Living with Fahr’s Syndrome: Coping Strategies and Support
The journey of living with this condition is undoubtedly challenging, but it is marked by the resilience of individuals and their support networks. Patients and their families often embark on a path of adaptation, finding solace in various coping strategies.
Embracing a healthy lifestyle, engaging in mental stimulation, and connecting with support groups can empower both patients and caregivers to navigate the complexities of this rare condition.
Prevention and Future Research on Fahr’s Syndrome
Preventing this condition remains a complex task due to its multifactorial nature. However, early detection of risk factors and genetic markers could potentially pave the way for personalized interventions that delay or mitigate its onset.
Research efforts are ongoing to unravel the underlying mechanisms of the disease, with advancements in genetics and neurology offering hope for breakthroughs in treatment and prevention strategies.
Conclusion
Fahr’s Syndrome, though shrouded in mystery, is slowly unveiling its secrets to the diligent efforts of medical researchers and the unwavering determination of those affected. As science inches closer to understanding its origins and mechanisms, the doors to improved treatments and enhanced support swing open.
By fostering awareness, embracing innovation, and uniting in the face of adversity, we can illuminate the path towards a brighter future for this patient’s condition and their loved ones.

